Call Us : +1 (626) 798-0558

What to Expect During Short-Term Rehab After Surgery in Pasadena
Short-term rehabilitation after surgery is a structured, medically supervised recovery program that helps your loved one regain strength, mobility, and independence before returning home. It typically begins within 24 to 72 hours of hospital discharge and lasts anywhere from a few days to several weeks, depending on the procedure and your loved one’s progress. If a surgeon or hospital discharge planner has recommended a skilled nursing facility for recovery, this page explains exactly what that process looks like.
Why the Hospital Sends Your Loved One Somewhere Else First
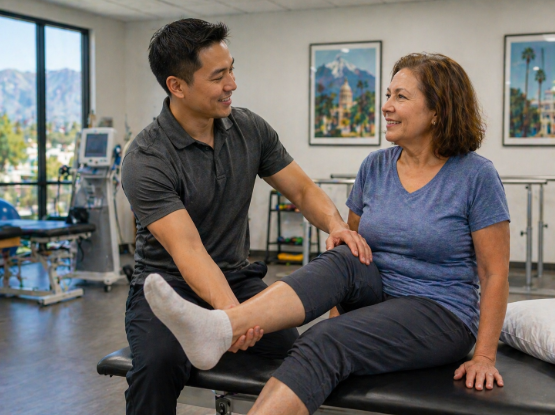 Hospitals prioritize stabilization. Once the surgical team has managed the acute phase, the focus shifts to recovery, and hospitals are not set up for that. Skilled nursing facilities fill the gap between hospital discharge and a safe return home.
Hospitals prioritize stabilization. Once the surgical team has managed the acute phase, the focus shifts to recovery, and hospitals are not set up for that. Skilled nursing facilities fill the gap between hospital discharge and a safe return home.
The transition can feel abrupt. One day, your loved one is in a hospital bed, and the next, you are being asked to make a placement decision quickly. That pressure is real, and it is worth understanding what the facility actually provides before you sign anything.
Short-term rehab at a skilled nursing facility typically includes daily therapy sessions, 24-hour nursing supervision, medication management, wound care if needed, and ongoing coordination with the attending physician. The goal is not long-term placement. The goal is a safe, complete recovery.
What Happens on Day One
Arrival at a skilled nursing facility is not passive. Within the first 24 hours, your loved one will receive a full clinical assessment. The care team reviews the hospital discharge summary, evaluates current functional status, identifies fall risk, assesses pain levels, and documents any wound or incision that needs monitoring.
From that assessment, a personalized care plan is built. This plan determines how many therapy sessions per day your loved one will receive, which disciplines are involved, what the goals are, and what milestones signal readiness to go home.
Family members are included in this process. You can ask questions, request copies of the care plan, and confirm that the goals reflect what your loved one actually wants from recovery.
The Three Types of Therapy Involved in Post-Surgical Recovery
Most short-term rehab stays involve one or more of three therapy types. The combination depends on the procedure and where the functional deficits are.
Physical therapy addresses mobility, strength, balance, and pain. After a hip or knee replacement, this is typically the primary discipline. A physical therapist will work with your loved one on standing, walking, stair navigation, and safe transfers from bed to chair to bathroom. Sessions are typically 45 to 60 minutes and occur once or twice daily in active recovery phases.
Occupational therapy focuses on the activities of daily living: bathing, dressing, grooming, cooking, and managing the home environment safely. After a cardiac procedure, stroke, or any surgery affecting the upper extremities, occupational therapy becomes central to the plan. The OT often conducts a home safety assessment before discharge to flag hazards like loose rugs, missing grab bars, or staircases that need to be addressed.
Speech therapy is less commonly required after orthopedic surgeries but is frequently part of recovery following stroke, neurological events, or surgeries involving the head, neck, or airway. Speech therapists address swallowing difficulties, communication, and cognitive function that affect safe, independent living.
How Long Short-Term Rehab Actually Lasts
There is no single standard length of stay. Recovery timelines depend on the procedure, pre-surgical health status, age, and how quickly your loved one responds to therapy.
As a general reference, the Centers for Medicare and Medicaid Services reports that the average skilled nursing facility stay for Medicare beneficiaries is approximately 27 days, though many post-surgical stays are shorter. A straightforward hip replacement in an otherwise healthy adult may result in a 10 to 14-day stay. A more complex cardiac recovery or a procedure involving significant deconditioning may extend to 30 days or beyond.
Progress is evaluated weekly. If your loved one is meeting goals ahead of schedule, discharge planning can begin early. If recovery is slower than expected, the team will document the clinical justification for continued stay, which is required for ongoing Medicare coverage.
Medicare Coverage for Short-Term Rehab After Surgery
 Medicare Part A covers short-term skilled nursing facility care under specific conditions. Your loved one must have had a qualifying hospital stay of at least three consecutive inpatient days. The admission to the skilled nursing facility must occur within 30 days of the hospital discharge. And the care required must be skilled, meaning it needs the involvement of licensed nurses or therapists, not just custodial assistance.
Medicare Part A covers short-term skilled nursing facility care under specific conditions. Your loved one must have had a qualifying hospital stay of at least three consecutive inpatient days. The admission to the skilled nursing facility must occur within 30 days of the hospital discharge. And the care required must be skilled, meaning it needs the involvement of licensed nurses or therapists, not just custodial assistance.
When those conditions are met, Medicare covers the full cost of days 1 through 20. For days 21 through 100, there is a coinsurance amount. In 2024, that coinsurance was $194.50 per day, according to Medicare.gov. Beyond day 100, Medicare coverage ends, and other payment sources apply.
Medi-Cal may cover skilled nursing care for eligible residents, including coverage that extends beyond the Medicare benefit period. Eligibility and benefit structure vary. The facility’s admissions team can review your loved one’s coverage at intake and connect you with a benefits counselor if needed.
For authoritative coverage details, the official Medicare resource is Medicare.gov’s skilled nursing facility coverage guide.
What a Typical Day in Short-Term Rehab Looks Like
Structure matters in recovery. Consistent daily routines reduce anxiety, support healing, and make progress measurable. A typical day in short-term rehab is built around therapy sessions, with meals, rest, nursing check-ins, and personal care woven around them.
Mornings typically begin with breakfast, personal care assistance if needed, and a review of the day’s therapy schedule. Physical or occupational therapy sessions often run mid-morning. Lunch is followed by a rest period, then a second therapy session in the afternoon. Evenings are quieter: dinner, medication administration, and time for family visits.
Nursing staff monitor vitals, wound healing, pain levels, and any changes in condition throughout the day and overnight. This continuous oversight is what separates skilled nursing from home recovery or assisted living. Someone is always present and trained to respond.
What Signals That Your Loved One Is Ready to Go Home
Discharge from short-term rehab is not a calendar decision. It is a clinical one. The care team assesses whether your loved one can safely perform the tasks required at home, with or without support. That includes walking safely on different surfaces, getting in and out of bed independently or with planned assistance, managing personal care, and understanding medication instructions.
The occupational therapist’s home safety assessment plays a significant role here. If the home environment presents risks that cannot be addressed before discharge, the team will flag that and work with your family to find solutions, whether through equipment, home modification, or transitional home care services.
Families sometimes feel pressure to take their loved one home before the clinical team believes it is safe. That pressure is understandable but worth resisting. Premature discharge is a leading cause of hospital readmission after surgery. The recovery window is finite. Using it fully is almost always worth it.
Choosing a Short-Term Rehab Facility in Pasadena
 Location matters more than most families initially expect. A facility close to home makes family visits realistic, which research consistently links to better outcomes and shorter stays. The short-term rehabilitation program at Pasadena Nursing Center is located in Pasadena at 1570 N Fair Oaks Ave, placing it within close reach of families throughout the San Gabriel Valley.
Location matters more than most families initially expect. A facility close to home makes family visits realistic, which research consistently links to better outcomes and shorter stays. The short-term rehabilitation program at Pasadena Nursing Center is located in Pasadena at 1570 N Fair Oaks Ave, placing it within close reach of families throughout the San Gabriel Valley.
When evaluating any facility, ask specifically about therapy frequency. Some facilities offer therapy five days a week. Others offer seven. For an active post-surgical recovery, more frequent sessions accelerate progress. Ask what happens on weekends. Ask whether therapy is provided by facility staff or contracted out. Both models exist, and both can work, but you deserve a clear answer.
Also, ask about physician involvement. A facility with an attending physician or medical director who visits regularly provides a different level of oversight than one that relies entirely on telephone consultations.
Frequently Asked Questions
How soon after surgery does short-term rehab begin?
Most short-term rehab placements occur within 24 to 72 hours of hospital discharge. The hospital discharge planner coordinates the transfer, and the receiving facility typically completes an intake assessment on the same day of arrival. Therapy often begins the following morning.
Can my loved one return home directly after surgery instead of going to rehab?
In some cases, yes. Patients with strong pre-surgical health, reliable home support, and less complex procedures may be discharged directly home with outpatient therapy. However, when a surgeon or hospital recommends a skilled nursing placement, it reflects a clinical judgment that the recovery needs exceed what can be safely managed at home. That recommendation is worth taking seriously.
Does Medicare cover the full cost of short-term rehab after surgery?
Medicare Part A covers 100 percent of approved costs for the first 20 days of a skilled nursing facility stay, provided the qualifying hospital stay and admission timeline requirements are met. Days 21 through 100 require a daily coinsurance payment, which was $194.50 per day in 2024. Coverage ends at day 100. Medi-Cal and supplemental insurance may cover costs beyond that point for eligible residents.
What is the difference between short-term rehab and long-term care?
Short-term rehab is goal-oriented and time-limited. The plan is built around specific recovery targets, and the expectation is that your loved one will return home or transition to a lower level of care once those targets are met. Long-term care is for individuals who require ongoing nursing supervision and assistance with daily living that cannot be safely managed at home. Some residents begin with short-term rehab and transition to long-term care if their needs are greater than anticipated.
Can family members visit during the short-term rehab stay?
Yes. Family involvement is encouraged. Visiting during therapy sessions, when permitted by the therapy team, gives families a direct view of progress and helps with discharge planning. Most facilities have designated visiting hours, though policies vary. Pasadena Nursing Center welcomes family participation in the care process.
What should I bring to the facility on admission day?
Bring insurance cards, a current medication list with dosages, a photo ID, comfortable clothing suitable for therapy, non-slip footwear, and any personal comfort items your loved one wants. Bring a list of questions for the admissions and nursing staff. Ask specifically about the care plan timeline, therapy schedule, and how family members will receive updates on progress.
Taking the Next Step
If your loved one’s surgeon or hospital has recommended a skilled nursing placement for post-surgical recovery, the decision timeline is often shorter than families expect. Knowing what the rehabilitation process looks like, what Medicare covers, and what questions to ask puts you in a far better position to choose the right facility quickly and confidently.
Pasadena Nursing Center at 1570 N Fair Oaks Ave has supported families across Pasadena, Arcadia, San Marino, Temple City, Alhambra, Monrovia, and Sierra Madre through post-surgical recovery. If you have questions about the short-term rehab program or want to arrange a visit before a decision needs to be made, call (626) 888-8203.
Pasadena Nursing Center
1570 N Fair Oaks Ave, Pasadena, CA 91103
Phone: (626) 888-8203
